Welcome to My Blog
Recipes, Tips, & More
Histamine Intolerance 101: Foods, Symptoms, and How It’s Managed
Histamine intolerance has become a popular explanation for a wide range of vague and frustrating symptoms, especially those affecting the gut, skin, and nervous system. Many people who suspect histamines are to blame report issues like bloating, headaches, flushing,...
Diverticulosis vs. Diverticulitis: What’s the Difference and How to Manage Both
Many people are diagnosed with diverticulosis during a routine colonoscopy and are unsure what it means. While the terms sound similar, diverticulosis and diverticulitis are very different. While both conditions involve the colon, they differ in inflammation and...
Food Chemical Sensitivity: What It Is and How To Manage, According To a Dietitian
Have you ever eaten a perfectly normal meal, only to feel bloated, foggy, or unwell hours later, wondering if hidden "food chemicals" might be to blame? More and more people are asking this question as awareness around food chemical sensitivity grows. Unlike an...
How Menopause Affects Gut Health – And What You Can Do About It
Menopause marks the natural end of a woman's reproductive years. Typically occurring between the ages of 45 and 56, it's defined as going 12 consecutive months without a menstrual period. Menopause is often accompanied by a range of physical and emotional changes,...
The Gut-Skin Connection: How Your Microbiome Shapes Clear, Healthy Skin
If you've ever suspected that your gut health influences your skin issues, you're not imagining things. New research has started looking at the gut-skin connection—the idea that the health of your digestive system directly affects the health of your skin. From acne...
The Scoop on Poop: What’s Normal, What’s Not & How to Improve Your Gut Health
Poop—it's not the most glamorous topic, but it's a crucial indicator of your overall health. Your digestive system is important for breaking down food, absorbing nutrients, and eliminating waste, so when something is off with your gut, your poop will likely reflect...
The Vagus Nerve and Health: What’s the Connection?
The vagus nerve is a powerful piece of the body's communication network, linking the brain to various essential systems like the heart, lungs, and gut. It plays an important role in the autonomic nervous system, helping regulate involuntary functions such as heart...
The Link Between the Gut Microbiome and Mental Health
When it comes to health, many people think of the mind and body as separate entities. However, in the last few decades, scientists have been uncovering a powerful connection between the gut and the brain. Emerging research shows that the health of your gut...
Wheat and Digestive Symptoms: Is It Gluten or Something Else?
In recent years, gluten-related disorders have gained significant attention, leading to a surge in people following gluten-free diets and new gluten-free products on store shelves. This has been driven by the increasing number of people experiencing digestive problems...
Unlocking the Health Benefits of Short Chain Fatty Acids (SCFAs)
Short-chain fatty acids (SCFAs) are a type of fatty acid produced when dietary fiber is fermented by your gut microbes in the large intestine. Despite their small size, SCFAs play a significant role in maintaining overall health. Primarily composed of acetate,...
Exploring the Link Between Weight and the Gut Microbiome
Research into the gut microbiome has exploded in recent years, revealing its significance in various health conditions, including obesity, inflammatory bowel diseases, allergies, and even neurological disorders like Parkinson's disease and autism spectrum disorders....
Understanding Metabolic Endotoxemia: The Link Between Diet, Gut Health, and Chronic Disease
Metabolic endotoxemia is a condition where harmful substances called lipopolysaccharides (LPS) from the gut bacteria enter the bloodstream. This occurs due to changes in the gut caused by certain dietary and lifestyle factors. The entry of LPS into the bloodstream can...
Exploring the Link Between Cannabis Use and Gut Health
Cannabis is gaining increased attention for its potential health benefits. However, there is still a lot we don’t know about cannabis, so it can be hard to make specific recommendations for its use. One area of growing interest is the effect of cannabis on gut health....
Does Sugar Cause Inflammation and Pain? Everything You Need to Know
Does Sugar Cause Inflammation and Pain? Everything You Need to Know Inflammation is an important part of the immune response, but when it becomes chronic, it can lead to the development of chronic diseases such as obesity, type 2 diabetes, and heart disease. Sugar is...
The Gut Check: Unraveling the Effects of Alcohol on Gut Health
While enjoying a social drink occasionally likely isn’t cause for alarm, excessive alcohol intake carries several health risks, including high blood pressure and various cancers. But what about the effect of alcohol on the gut? While we’re still learning about the...
Celiac Disease Self-Care
If you’ve been diagnosed with celiac disease, you’re probably familiar with the gluten-free diet. For people with celiac disease, following a gluten-free diet is an essential part of managing the disease. But the gluten-free diet is quite restrictive, which can lead...
Alternative Therapies for IBS
Alternative Therapies for IBS IBS is highly individual, and the treatment that works for one person may not work for another. This has led to a growing interest in the use of alternative therapies for IBS. From herbs for IBS to gut hypnotherapy, there are many...
Dyssynergic Defecation and Pelvic Floor Therapy for Constipation: What You Need to Know
Have you made changes to your diet but are still struggling to go? If so, you may have a condition called dyssynergic defecation. Dyssynergic defecation is a condition where your pelvic floor does not properly coordinate the nerves and muscles, making it difficult to...
Your Constipation Care Plan: Natural Remedies for Constipation
Feeling stuck? Constipation is a common medical problem, yet many people don’t seek help for it. Luckily, there are several natural remedies that you can use to improve constipation. Read on to learn how to create your own constipation care plan using natural remedies...
Breast Implant Illness
When I became a dietitian, I had no idea the profound effect food could have on the body. It wasn’t until I started to get more into the functional/integrative side of nutrition that I realized the powerful impact of the combination of food and supplements. I have...
What Is the Low FODMAP Diet?
Have you or anyone you know ever had digestive issues? Most of us would probably answer “yes” to that question; we’ve all had days where we haven’t eaten very well or we’ve over-indulged (I’m looking at you, Thanksgiving) and our stomachs have paid the price the next...
Lemon-Dill Butter Chicken
A short story behind this recipe. The last time we went to visit my mom she made us this chicken dish. My aunt had made it for her and she liked it so much she asked for the recipe. So, to make a long and kind of boring story short, I do not have anyone to give credit...
Why a Prokinetic?
Each year that I have been in practice, the more clients I see with small intestinal bacteria overgrowth (SIBO). When I opened my business over 3 years ago, SIBO was not a term in my vocabulary. I honestly don’t remember where and when I first heard about it....
Why do I need to rush to the bathroom after a meal?
Over the years of being a GI dietitian I have joined many of the FODMAP Facebook groups for more information to help my clients. One question I see posted often is about the need to rush to the bathroom soon after a meal. These individuals ask this because it is felt...
Basic FODMAP Friendly Bread
I love just plain basic bread. I no longer eat gluten and I like try different paleo recipes. The problem is that many of the recipes I do use, my clients have trouble with some of the ingredients. When I come across a recipe I really like, I look to modify it to be...
In a Rush Zucchini/Spinach Muffins
I am always looking for something different to eat for breakfast. I'm not one of those that can eat the same thing every day, so I look for variety in my meals and snacks. Plus, I often need something that I can just grab and bring with me. Recipe: -2 cups grated...
Focusing on YOU with a food related diagnosis
Many of my clients comment that co-workers, friends and even sometimes family are not understanding of their diagnosis or why they are eating a certain way. It is difficult to be in social settings with food and feel like you aren't eating like everyone else, or able...
Banana Chocolate Chip Muffins
I promise I won't just post muffin recipes. They are just one of my favorite quick foods for breakfast or a snack. Ingredients: -1/2 cup sugar -2 bananas* -2 eggs -1/2 cup oil (your choice what type) -2 cups spinach -1 1/4 cup almond flour** -1 cup gluten-free oats***...
A Middle Schooler can get IBS too!
I asked the mother of one of my clients if she would like to write about her son's journey with IBS. Below is a very condensed version of his story. Some people are "fixed" quickly, while others, the pieces of the puzzle take a lot longer to fall into place. This...
How Getting a Great Sleep Helps You Make Healthy Choices
When you're tired, everything is more difficult, and that includes making good food choices. Sleep deprivation can interfere with your self control, appetite, metabolism, and cravings. When you get enough sleep, it's easier to make good nutrition choices. You have...
Have you ever heard of NAFLD?
When I attended the University of Michigan Conference this fall, one topic they presented on was Non-Alcoholic Fatty Liver Disease (NAFLD). This disorder is when there is an accumulation of fat in the liver of an individual, but they do not consume much alcohol. There...
How Big of a Problem is Accidental Gluten Exposure?
Many individuals follow a gluten-free diet for various reasons. An individual could have a celiac diagnosis, wheat allergy, gluten sensitivity, leaky gut, or even IBD, such as Crohn’s or Colitis. Many of the diets for various disease states take gluten off the menu,...
Still searching for an answer to your symptoms?
Over my years as a dietitian, I have seen many individuals struggle with various symptoms. Even while working at Johns Hopkins, there were some they just couldn't quite figure out what was going on. I was always under the impression that if you go to the doctor, you...
Modified Your Way Shepherd’s Pie
I feel like Shepherd's Pie is so versatile. No matter what eating plan an individual follows, this dish can usually be modified to meet someone's needs. I also like that it is fairly quick to make and healthy. This is the recipe I made, but I will also throw out...
How To Use Food For Better Sleep
The battle for sleep is real. With the right nutrients, you can give your body the fuel it needs to function properly and get a full seven to nine hours of sleep every day. Fuel Your Body RightFoods contain the nutrients your body uses to make sleep hormones like...
Blueberry Bars
This recipe was adapted from blogger, Katalyst Health at katalysthealthblog.com. I added ingredients to increase the nutrition of the bars. This is one of my favorite recipes. It is easy to make and yummy! This is a paleo recipe, but can be adapted to fit your...
Client Story of IBS/FODMAP Diet
I've suffered from IBS-C since I was 6 years old but I wasn't officially diagnosed until I was 26 or 27. I thought it was normal to be constipated. Throughout childhood, teenage years, and early twenties, primary care and family doctors would instruct me to drink more...
Is it Lactose Intolerance or A1 Beta-Casein Protein Intolerance?
What is Beta-Casein? Beta-Casein is a protein found in cows’ milk. There are two types of beta-casein in conventional milk, A1 and A2. A2 is said to be the original variant, as it existed prior to the appearance of A1. Regular cows’ milk in the US contains a mix of A1...
What is Congenital Sucrase-Isomaltase Deficiency (CSID)?
I attended a three day GI conference at the University of Michigan in September. It was an amazing conference packed full of presentations from some of the best GI doctors and dietitians. One presentation was on a topic I had never heard of, so I was intrigued and...
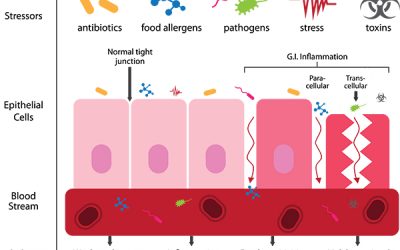
Is There Really Such Thing As Leaky Gut?
Is There Really Such Thing As Leaky Gut? Sometime during 2015 I was told I had “leaky gut.” I had no idea what it meant or if it was an actual diagnosis. I had not heard the term in college or any of my time working at Johns Hopkins Hospital. In December 2016, I was...